Key Drivers of Remote Patient Monitoring (RPM) Adoption in 2021
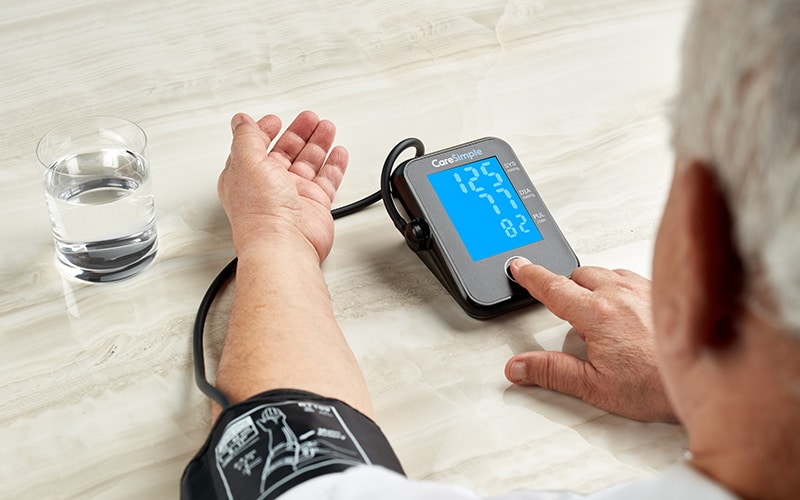
Remote patient monitoring (RPM) rewards patients, providers and payers alike. The technology allows physicians to keep their patients’ health under control while at home, digitizes the physician/patient relationship, generates new recurring revenues for their practices and helps to lower overall healthcare costs. As a result of this, it’s no surprise that RPM adoption is growing fast. In fact, 33% of physicians who weren’t using RPM in 2020 are planning to integrate RPM into their practice over the next year, and it is projected that the global RPM systems market will be worth over $1.7 billion by 2027.
What’s causing this uptick in RPM adoption? CareSimple sees a number of drivers making an impact:
COVID-19 Pandemic
While RPM has been around for some time now, the pandemic quickly brought the concept of virtual health monitoring back to the forefront. COVID-19 led to many people quarantining at home to reduce/avoid exposure to the virus, while also creating an urgent need for hospital capacity and clinical resources. While in recent years, the Centers for Medicare and Medicaid Services (CMS) had designated new reimbursement codes to make RPM more accessible, COVID brought about additional changes that allowed providers to use RPM for patients with acute and chronic conditions, whether it be for new or established candidates.
Using RPM, healthcare providers were able to expand care beyond the four walls of a hospital. For patients that tested positive for COVID-19 and were able to safely quarantine at home during recovery, RPM enabled providers to still monitor vitals such as blood pressure and blood oxygen levels, while also minimizing the risk of spread and exposure to the virus. RPM also benefited non-COVID patients who required chronic care, like seniors, providing peace of mind that conditions could be remotely monitored from the comfort and privacy of their own homes. This in turn freed up beds and clinical resources at hospitals and healthcare facilities for patients that required in-person immediate care.
Prevalence of Chronic Diseases
According to the CDC, six in 10 adults in the United States have a chronic disease, and four in 10 have two or more. With that, 86% of U.S. health expenditures are attributed to people with chronic medical or mental health conditions. Not only is this burdensome on the patients with these diseases who require frequent care, but it is a major onus on the nation’s healthcare system and its providers. To help manage this influx of chronic diseases, RPM is a great tool for managing conditions such as hypertension, chronic obstructive pulmonary disease (COPD), diabetes, congestive heart failure (CHF) and more.
Patients with co-morbidities often need daily tracking of blood glucose levels, blood pressure, nutrition management, etc., to ensure they are maintaining and managing their disease state well. With RPM, patients can use medical devices at home to take their vitals as prescribed, and this data can be sent in near real-time to their clinicians and integrated directly into the electronic health record (EHR). This approach provides healthcare providers with a more holistic view of their patients’ health, and increased visibility into when patient data is out of a normal range or trending in the wrong direction. As a result, care is streamlined for patients, and providers can intervene more quickly, thus significantly improving patient outcomes and lessening chance for readmission. A KLAS Research report that surveyed 25 healthcare organizations found 38% of healthcare organizations running RPM programs focused on chronic care management reported reduced admissions, and 17% cited cost reductions.
Demand from Patients
In recent years, the benefits of RPM became commonly accepted among the professional community, but little evidence existed on one of its potentially biggest challenges: patient buy-in.
With a recent study from MSI International revealing that 4 out of 5 Americans view remote patient monitoring favorably, and more than 60% of respondents open to sharing their blood pressure, heart rate, blood sugar and blood oxygen data, payers and providers can now confidently move forward knowing that patients share their enthusiasm for RPM and are willing to give it a chance to improve their health.
Simplicity
As mentioned, RPM is not an entirely new offering, but to date has typically been associated with its own set of integration and execution challenges, with organizations dealing with purchasing hubs, provisioning tablets, pairing peripherals, a complex setup process for patients, connectivity barriers and hours spent on technical support. There has also been a resistance to adopt RPM due to the changes it brings to existing clinical workflows.
RPM need not be a complicated undertaking, rather it can be quite simplistic, further promoting adoption of the technology to remotely engage any patient. At CareSimple, we provide pre-configured medical devices that work directly out-of-the-box, with no pairing, WiFi, or setup required. For patients, the ease of use means they can take control of their health, gathering their data from cellular-enabled devices, which then automatically transmit the data to the healthcare provider. For providers, the technology blends with 1:1 care to create an engaging experience that works for everyone – physicians, care managers, patients, etc. Care teams receive vitals and patient data in near real time, managing patients from a single portal that can be integrated into the EHR. This approach simplifies the process of integrating RPM into clinical workflows so it can be prescribed to patents for a variety of use cases, from ambulatory care, post-acute and large-scale clinical studies.
Interested in learning more? Contact us to have our specialists provide a personalized walk-through of CareSimple’s RPM platform.